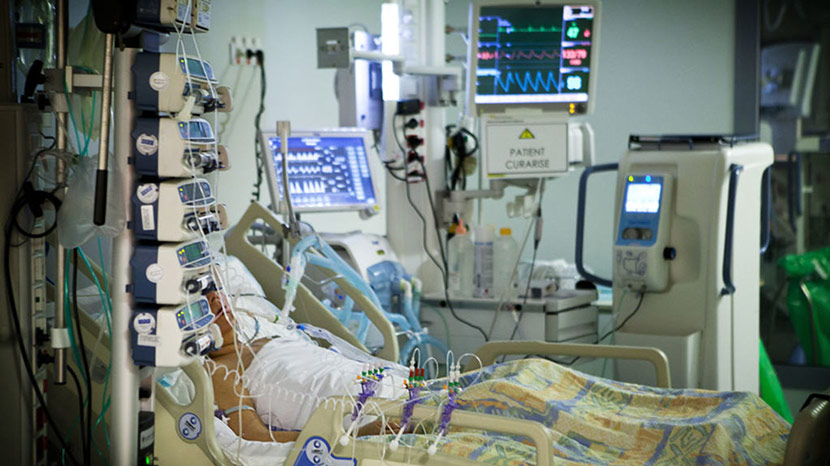
For today’s GeriPal Podcast we talk with Drs. Nathan Brummel and Lauren Ferrante, both critical care physician-researchers, about integrating geriatrics principles in intensive care units.
This is a major issue. Just think about the older patients you’ve seen in the ICU recently: older, frail, sick. Now imagine the environment – beeping, monitors, lines (tethers), sedating medications, stress, open doors, lights everywhere, noisy air mattresses. The environment alone is crying out for geriatricization! (I think I just made up a word).
Nathan and Lauren wrote a terrific article about the topic, link below, and discuss the landscape of work to be done in this area on this podcast.
Enjoy!
-Alex Smith, @AlexSmithMD
Link:
Eric: Welcome to the GeriPal podcast. This is Eric Widera.
Alex: This is Alex Smith.
Eric: And Alex, we have two guests with us. One’s skyping in and one here in studio.
Alex: Let’s start with the in-studio guest. We have Nathan Brummel who is a Pulmonary Critical Care Physician Researcher at Vanderbilt and is in town for the GeriPal podcast and also happens to be attending the American Delirium Society meeting which is in San Francisco.
Eric: Great. I was just there yesterday. Great meeting.
Nathan: It is. It is.
Alex: Welcome to GeriPal podcast Nathan.
Nathan: Thanks for having me.
Alex: We also have via Skype Lauren Ferrante who is a Pulmonary Critical Care Physician Researcher at Yale. Welcome to the GeriPal podcast Lauren.
Lauren: Thanks for having me.
Eric: Lauren, we ask all of our guests, do you have a song request for Alex?
Lauren: Yes. We wanted to sing a song about change and so we are requesting “Waiting on the World to Change” by John Mayer.
Alex: Alright.
Alex: We keep on waiting … Wait, let’s do that again. Eric, you’ve got to sing too.
Eric: I have to sing too?
Alex: Yeah. You’ve got to sing “waiting”.
Eric: Alright.
Alex: Yeah. We need it. We need the backup. Let me start again. [Singing]
Alex: Alright!
Eric: I can’t believe you made me sing, Alex.
Alex: It’s great. That song is actually about how you’re waiting for others to change. Is that what you’re advocating here when you’re thinking about geriatricizing ICU’s? Should we be waiting for them to change themselves? Is that the point?
Lauren: No. The whole point of the article is that we are advocating that the time for change is now.
Eric: Wait. What article are we talking about, Alex, here?
Alex: We should say that the topic of today is geriatricizing the ICU which is like critical care medicine. The title of the article is “Integrating Geriatric Principles Into Critical Care Medicine: The Time Is Now”. And this was in Annals of the American Thoracic Society recently May of this year. Nathan and Lauren were both authors on this. Eric, do you want to start us off with the discussion here?
Eric: Yeah, so we’ll have a link to this article online on our GeriPal blog. We usually like to start off how did both of you get interested in this subject?
Nathan: Sure. It started about three years ago at the American Geriatric Society meeting. There’s a medical sub specialty section and at that breakfast Lauren and I were sitting together, we’re both pulmonary critical care and knew each other through that but were at the AGS meeting. All the other groups were getting up, the cardiology section, the oncology section and they were presenting all the great work they were doing. We both sort of looked at each other and said, “Why not us?” We need something like this in critical care.
From that rose a sort of discussion between Lauren and I. We then put together an application to become a working group in the American Thoracic Society, the largest international group of pulmonary critical care physicians. Over the last few years that’s morphed into an interest group now so we have a larger group that’s working to do these very things of integrate geriatrics and aging research into critical care medicine.
Alex: Lauren, anything to add to that about like why did you see this as necessary? It was certainly a need there. Anything from your clinical experience that sort of cries out for this area?
Lauren: Definitely. I think in the hospital and in the medical schools we all talk about integration but we still tend to function in silos even in the ICU where we have to manage every single organ system. Actually, the ICU is pretty good at interdisciplinary and multidisciplinary care but with the growing number of older adults in our country and this is something that’s been talked about a lot including on this podcast. I think we really saw that it’s time to integrate these principles and not just to be calling geriatrics consults all the time. That’s one of the things we address in the article.
Although we’re both researchers, really it was the clinical need for this and that kind of drove us to form this working group and to address all facets of integrating geriatrics into critical care research education and clinical practice.
Eric: When we talk about principles, what geriatric principles are we actually talking about here?
Lauren: We’re talking about a number of things. One of the things that both Nate and I have worked on are vulnerability factors that are present to a greater extent among older adults than they are among younger patients. These include things like frailty, or multi-morbidity, or cognitive impairment, or disability. And, many older adults are coming into the ICU with these preexisting problems but when we’re looking at the critically ill older adult patient, it’s extremely rare for someone in the ICU to be thinking about that at the forefront of their mind. We tend to focus on things inherent to the critical illness itself so something like respiratory failure that’s keeping them on the vent and we’re not really thinking about what they’re coming in with. That’s just one example.
Where a geriatrician might be thinking first about the preexisting vulnerability factors that an older adult is coming into the hospital with and how those vulnerability factors might inform their outcomes or their acute illness. That’s just one example of a principle or at least consideration that we think we need to integrate into our practice that really isn’t being considered in real time in the ICU currently.
Nathan: Yeah and I think adding to that, the increased emphasis on outcomes after critical illness. We’re seeing things that are classically considered geriatric syndromes like cognitive impairment, disability and frailty in even our younger survivors. There’s an added component not only for the older adults but younger survivors who are suffering with classic geriatric syndromes.
Alex: Of the geriatric syndromes, what do you think is the most common in the ICU? The one that comes to mind for me, well, it was sort of primed for this, was delirium. Does that ring true to you or is there actually empirical evidence about what’s most common?
Nathan: Yeah. We haven’t studied specifically the types of geriatric syndromes but delirium being the most common affecting up to 80% of people that are on a mechanical ventilator.
Alex: Wow. Say that again.
Nathan: Up to 80% will have at least one day of delirium while they’re in the ICU.
Alex: Wow. That’s huge.
Nathan: That cuts across ages and comorbidities and all these other factors. The vulnerability factors plus the insult that critical illness is that brings those two together. I think the other one that’s ubiquitous is immobility.
Lauren: Yes definitely.
Nathan: Every single patient in the ICU is even though we’re trying to get better at that, it’s still quite common.
Alex: What sort of … What do you think is, there are a couple of historical factors we start to get into this here a little bit. The ICU has changed over time, right? It used to be younger folks with reversible conditions, right? One of my mentees, Brian Block who I think both of you have met is writing a piece where he talks about how that ICU has really changed from being a place where young people with polio were on ventilators and now it’s just replete with older adults, dementia often, other geriatric conditions. The demographics and the illnesses and conditions that are seen in the ICU have really changed over time.
Nathan: Right. That’s a combination of things. One is that the population is aging but two is this is the population that’s most likely to develop common reasons for ICU admissions, thinks like sepsis and pneumonia and respiratory failure. All of those track with age as well. I think another factor as well is it’s not as socially acceptable to deny older adults ICU admission like it once was.
Alex: Lauren, from your perspective, thinking about the level of expertise and awareness of the importance of this issue within the American Thoracic Society, within critical care physicians nationwide or even globally, where do you think we’re at? Is this a frontier area or do they recognize it’s important they have a need? Do they already have some training? Or is this pretty new stuff to them?
Lauren: I think that there is increasing awareness of the need and if you look back even I think it was Derek Angus back in 2000 had looked at the epidemiology and the prevalence of older adults in the ICU. We mentioned that in our article. At the time, he found that more than half of patients in the ICU were older adults.
If you look at, this is not an official publication research project that I did, but if you look generally at the number of citations and interest in this area, it has been increasing since that time. And, in fact, there’s decent interest in mid career senior folks and also in early career investigators in these specific issues. And the group that Nate described that we created in the American Thoracic Society has only grown and we keep getting additional interests from other ATS members. I just think that this is a really growing area and it is a frontier as far as incorporating these areas into practice. I think that we have seen a lot of progress in research, but we need to see the same amount of progress in clinical care and to continue the progress that we’ve made in research.
Eric: I’m just going to drill this down to practical issues of what we should be doing. There was a recent tweet that came out saying we have lots of tools for monitoring delirium in all age groups so what’s your excuse for not monitoring brain dysfunction?
Alex: Are you saying moderating?
Eric: Monitoring.
Alex: Oh monitoring.
Eric: Did I mispronounce that? Oops. There was an ICU doctor who had a rhetorical question. Is it important to monitor something for where there is no obvious intervention to make it better? The cam ICU suggest hypoactive delirium? What’s next?
Alex: Right. What do we do? We can detect it. What do we do about it? Interesting. Response?
Nathan: Yeah. I think it’s important that, I agree with that statement that we don’t have a drug that we can give which is what we all want. We want something quick and easy that we can give a patient. The problem or the difficult part about delirium is that you have to step back and stop and think about what might be causing it. The average ICU patient has upwards of 11 risk factors for developing delirium. Some of that is related to their underlying critical illness. We recently published a paper that looked at risk factors for delirium and we called them delirium subtypes and we identified a bunch of different like sepsis and hypoxemia and sedation was one of the ones that we looked at. We looked at the duration of each of those subtypes, each of those types of delirium. We found that each of them were related to long term cognitive impairment so delirium that people have in the ICU is related to their thinking and memory a year later.
What we found in that study was of all the causes, right, sepsis and hypoxemia, those don’t tend to be reversible but sedative associated delirium was associated with long term cognition. That’s a totally modifiable risk factor for delirium. It’s not necessarily giving something, it’s taking it away that may be helpful to patients. When you think of that, it’s important because it’s associated with outcomes but it’s also you can look for new problems that you can potentially intervene on.
Alex: Lauren it sounds like you wanted to add to that.
Lauren: Yeah. One of the things, one of the areas where we really can improve in the ICU and many units are working towards this, is the prevention of delirium. Some of the steps that we mentioned in our article include implementing interventions that are already pretty standard on ACE units or Acute Care for Elders units. These include things we mentioned additions and subtractions from the physical environment. Some additions to the physical environment might include portable amplifying devices for hearing impaired patients.
Alex: Yes.
Lauren: Those devices are not standard right now in Intensive Care Units. I usually find myself looking for one whenever I’m on service even though we have a pretty aging conscious unit here at Yale. Then other things would be subtractions from the existing environment. We all know that there’s a lot of sensory overload in the ICU and a lot of sleep disruption. Those things also predispose patients to delirium. I think we have a lot of work to do also in preventing ICU delirium in addition to treating it.
Eric: You did a nice job on your paper to break it down to things that we should be doing be doing now, things we should be thinking about short term in the next three years, and long term. Maybe we can briefly talk about each one of those. What should we be doing now to geriatricize ICU’s?
Nathan: I think the first thing is to start paying attention to these syndromes like delirium and immobility and sensory impairment that are prevalent. Those are modifiable right now. Eyeglasses, hearing aids, getting people up out of bed are interventions that are effective and by the way those at least mobility has been shown to reduce delirium in the ICU. That’s the only thing that we have to reduce delirium, two separate randomized control trials have shown that. The larger term or the more short term, the three to five years and five to ten year goals are things about educating more of the nuances of caring for older adults and treating geriatric syndromes in the ICU. Developing an educational curriculum, research, or research agenda, what gaps in knowledge do we have about caring for older adults? We actually submitted a proposal to review the literature and one of the comments we got back was well we all know there’s nothing there.
Alex: There is no literature.
Nathan: That’s our point.
Alex: Right. That’s the point. Lauren, do you want to add to that?
Lauren: Yeah. In addition to training pulmonary and critical care fellows to really consider these geriatrics principles especially as they become attendings, I also like to think a lot about what can we do with the current practitioners in the ICU. I saw a recent paper, I was just trying to find it, I think it was out at the UAB group where they talk about virtual ACE units and where they’re basically going around to different units and training the existing practitioners. I wonder if that might be a more practical model for early implementation.
Although we outline a number, I think one of the things we mention, just in service trainings, things like that. I think we can’t lose sight of the fact that we have to train our current practitioners so that they’re thinking about these concepts in real time.
The other thing that we mentioned for the future is we, and this is something Nate and I have talked about a lot is creating a network of aging intensivists researchers because one of the areas that we outline in the paper is that many clinical trials and studies in critical care medicine often exclude the oldest old or don’t have critical numbers of older adults. We’re hoping that our group which has a lot of critical care researchers in it will one day as we go from the K to the R phase will be able to have an aging intensivist network so that we can answer some questions about how to best treat older adults in the ICU.
Eric: Is there a reason for that lack of inclusion of oldest old into ICU research?
Nathan: From a practical perspective, it’s not that the study exclusion criteria, say if you’re over 85 or 90 you can’t be in this study, it’s that they exclude people with multiple comorbidities or cognitive impairment from their studies. They sort of de facto exclude older adults.
Lauren: Right.
Alex: Do you want to follow up on that Eric?
Eric: No. Go ahead.
Alex: It does seem like this is the bait and switch that often happens with clinical trials that they test it in a very select group of sort of healthier individuals in order to show efficacy but then they roll it out for people who have multi morbidity, dementia, functional impairment, real world oldest old type of patients and we have no idea whether it works in them or not. I love this idea of setting up a trials network to actually study this effectiveness in real world settings.
Lauren: And some of the, you know the demographics of the existing trials and near future trials may change now that the NIA’s mandating inclusion across the lifespan with that new policy which I think is going to be effective next year. But we still feel that there will be benefit to have this aging intensivist network. That’s in the longer term plan.
Eric: Right. Is there, you’ve probably been to a lot of ICU’s, is there a design element to ICU’s to make it more age friendly?
Alex: Are you talking about architecture?
Eric: Yeah. Like the way ICU’s are designed. I mean when we think about ACE units, it’s not just mobile ACE units but physical ACE units. A lot of times we also think about the design of those ACE units. Is there room for family members to be there? Is there room to actually do things like get up out of bed, walk around. Is there light coming in from the outside? Are the bathrooms easily accessible? What are your thoughts about that?
Nathan: I don’t know from a national perspective but at Vanderbilt about now gosh it’s when I was a fellow so it’s longer ago than I care to think about but when we opened a new critical care tower and that incorporated a lot of those things you just talked about. There’s space for the family to stay with the patient there. There is a bathroom that’s accessible. It’s a very large open space compared with our old ICU which you had to be an acrobat to be able to maneuver around all the equipment and the bed and everything like that. There may have been a chair in the corner for family versus a pull out couch or something for them to sleep on. I think those are important things.
We know from the demographic data that the number of ICU beds, even though the number of hospital beds nationally is decreasing, the number of ICU beds is increasing. Whether that’s conversion of existing hospital beds into ICU beds or construction of new ICU’s but I think that’s a very important point for hospital administrators and architects to keep in mind as they design these spaces to make them aging friendly.
Lauren: Yes. We also have a new unit at Yale so we also have, space is definitely not a problem, there are huge windows, lots of light. But there are some things inherent to the ICU that aren’t contingent on space that I think we, probably every ICU in the country, could improve on. And that one big problem is noise and also sleep disruption. We have a group here at Yale that works on sleep in the ICU. They measure the noise of the ICU and especially in certain rooms, it’s just because the monitors are outside in the hall it can be really, really disruptive to the patient and disorienting. You can see how that might predispose to delirium.
The other problem we still have in every ICU I think is a tethering problem. I often start talks that I give of a picture that I give of a patient in the ICU bed just so that the audience can really grasp what that looks like. There are telemetry wires, multiple lines, central lines, Foley catheters, sometimes CVVH and the tethering devices, despite our best attempts at early mobilization, they can still be problematic especially for older adult patients.
Alex: I think about our ICU, the monitors are in the room, there’s always at least one monitor beeping and if it’s not the monitor beeping, it’s the IV beeping, the fluids are beeping. There’s always a beep. There’s at least one beep if not two beeps. The television is on. They’ve got the air bed. And the air beds these days, the best air beds are wonderful for your skin but the decibel level of the air bed is like off the charts. You can hardly, I feel like I’m on an airplane with all that background noise. You need noise canceling headphones. We tried to have a meeting with an ICU patient the other day. We could hardly hear anything and we don’t have, we’re not like 88 years old with hearing loss. I can imagine just such deliriogenic, just sort of setting for older adults.
Nathan: It’s a harsh environment for sure, for sure.
Lauren: From a design issue, it should really not be that hard to have the alarms transmit outside or to the nurse somehow or on their mobile heart beat. All the practitioners in our units are now connected through iPhones. From a design standpoint, there’s really no reason that that alarm should be going off next to the patient’s head as opposed to on our personal device. Hopefully, we can break, maybe engineers need to start working on that.
Eric: Yeah. The medication pumps, those are the worst.
Lauren: Yes.
Eric: All around the hospital they just go off. They go off for about ten minutes before somebody can walk into the room and turn it off. I just know the little yellow silence button but that only lasts for like a minute.
Alex: Then you’ve got to push it again.
Lauren: Yes.
Eric: Is there anything else that you guys would like to talk about before we end?
Lauren: I have a question for both of you as geriatricians. You read our paper and you’ve seen that we think we need to integrate the principles of geriatrics into critical care medicine but we certainly want to keep our geriatric colleagues involved in the ICU. Do you think that this is a good idea integrating it? Do you think that it’s problematic from a geriatrics consult standpoint or do you think we would work together on this type of initiative? How do you foresee it from your end?
Eric: I love your analogy or the idea of bringing in an ACE unit into the ICU because if you look at a lot of ACE units, they’re not taking over care. They’re often just focusing on key geriatric syndromes for those individuals making recommendations on that. They don’t need to be heavily involved with every patient and sometimes it’s just a quick touch point. I can imagine the same thing happening in the ICU. I think the challenge is how do you actually staff that in hospitals. But I think if we think about interprofessional teams and ACE units, it’s a reasonable and attainable goal to actually get. You don’t have to do full geriatric consults on every ICU patient but you just develop a system where you can have those, even those quick touchpoints.
Alex: I just add to that to say that I think Eric, you’re in more touch with this data that I am. The number of fellows, geriatrics fellows, clinical geriatrics fellows has remained relatively flat.
Eric: It’s been relatively flat.
Alex: For a period of time. And there are a lot of older geriatricians who are retiring or approaching retirement age. I guess my point is there’s no way that there’s enough of a workforce of geriatricians to meet the demand in the ICU’s. And so the primary focus should be on primary geriatrics delivered by critical care physicians in the ICU and education of those physicians, changing the environment, education nurses and the whole interdisciplinary team.
Eric: Yeah. Part of me also thinks, I think we can harp a lot on that geriatric workforce issue and why things can’t happen. In some ways, that’s probably not where we want to start. We can make this change. The workforce is there. The workforce is there from a specialty geriatric standpoint. The workforce is there from a interprofessional geriatric standpoint. Again, if you’re in most ACE units, it’s not just the geriatrician. It is the nurse with geriatric expertise. It’s the physical therapist. It’s the pharmacist. It’s a team of individuals. And it’s also like you said making sure we are also educating great primary geriatric skills for ICU providers, again, not just physicians but the whole interprofessional teams. I do think the workforce is there. We can do this. It’s just getting bright people eager people, like the people we have on this podcast to actually make that change, not waiting.
Alex: Right. Don’t wait for the change.
Nathan: Be the change, be the change. I think you raise a very good point about that where Lauren and I and others around the country and around the world really are approaching this from a critical care perspective but I don’t know that we’ve really engaged our geriatrics colleagues to say hey let’s sit down and figure out what that primary geriatrics for the ICU really looks like and how do we train people in that. I think that’s a very good point that you raise.
Alex: One of our listeners out there or many of our listeners out there, if listening right now and you’re thinking to yourself “I want to get involved in this. I’m a geriatrician. I do a lot of consults in the ICU. I see the issues they’re talking about. This all rings true.” Contact Nathan, contact Lauren. Get involved. We need geriatricians to have input on this issue.
Eric: I think there’s a lot of great analogies. For instance like geriatric ED’s, emergency departments. Learning lessons from the places where this has been implemented both delivering specialty geriatric care and also in like geriatric ED’s, it’s a lot about primary geriatric care from physicians and nurses and everybody that’s involved and also design. Thinking about how we design these units whether ED’s, ICU’s, or hospitals.
Lauren: Absolutely and just to anyone who’s listening and is thinking I want to be involved, but I don’t know when I’m ever going to see an intensivist and I’m not going to the ETF meeting, we do have a group in the American Geriatric Society called the Medical Subspecialties Section and these are exactly the issues that we work on. If you email me or look in the program at the next AGS meeting, you should contact us even though the section is called the Medical Subspecialty Section, we actually invite everyone to come. Surgical subspecialists, geriatricians and these are the issues that we want to be talking about and working on. Again, that’s where this group started, the group that Nate and I formed was actually at that meeting.
Eric: Wonderful. Well I want to thank both of you for joining us at this GeriPal podcast.
Alex: Thank you Nathan. Thank you Lauren.
Nathan: Thank you Alex. Thank you Eric.
Lauren: Thank you.
Eric: And Alex, how about you end with a little bit more of that song.
Alex: [Singing]
Eric: No more waiting right, the change is now. I want to thank all of our listeners for joining us. We look forward to talking with you next week and thank you to our guests.
Lauren: Thanks for having us. This was fun.
Nathan: Thank you.
Alex: Thank you so much Lauren. Thanks Nathan. Appreciate it.



