 |
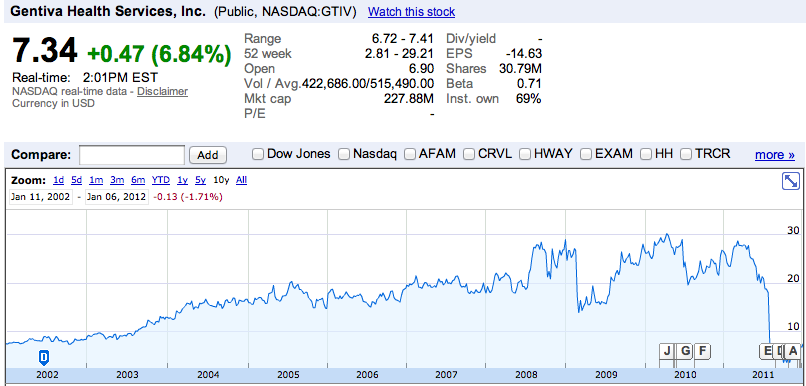
| 10 year stock price of Gentiva, the nation’s fastest growing for-profit hospice provider |
For-profit hospice has been in the news recently, and the press has not been favorable. We have this from a recent lengthy article in the Washington Post:
“Hospice care, once chiefly a charitable cause, has become a growth industry, with $14 billion in revenue, 1,800 for-profit providers and a base of Medicare-covered patients that doubled to 1.1 million from 2000 to 2009. Compensation based on enrollment numbers, pay to nursing-home doctors who double as hospice medical directors, and gifts to the nursing facilities have helped fuel the boom, according to a study of 1,000 pages of court documents and interviews with more than 45 hospice employees, patients and family members.”
And from Wednesday’s Kaiser Health News, we have:
“A national hospice company improperly cycled patients through nursing homes and hospice with a goal of making as much profit as possible from Medicare, according to a whistleblower lawsuit announced this week.”
All of this press on the heels of a terrific JAMA article by Melissa Wachterman and Ellen McCarthy at Beth Israel Deaconess Medical center that described differences between for-profit and nonprofit hospices. Seven percent of patients in for-profit hospices had lengths of stay of greater than one year, compared to three percent in nonprofit. For-profit hospices enrolled nearly twice as many patients with dementia – patients with lower skilled needs and longer lengths of stay.
 |
| St. Christopher’s Hospice, a nonprofit hospice established
by Cicely Saunders in 1967 |
And yet, for-profit hospices probably do some things that nonprofits don’t do well. The flip side of the above findings is that for-profit hospices are terrific at enrolling patients with advanced dementia, a terminal disease needing palliative care. For-profits tend to be larger, and because of the economies of scale associated with size, they’re able to provide more “open access” care to patients who are not yet ready to transition to an exclusively palliative approach. The argument can be made that most patients do not enroll in hospice long enough to realize the benefits. With this phenomena in mind, longer lengths of stay are a good thing – to a point – but where is that point? This is a central issue at stake.
What to make of all this? Is it possible to align the goals of outstanding end-of-life care with a for-profit model? Is it ethical?
One argument is to allow for-profit hospices to continue, but place better safeguards and do a better job of rooting out fraud and abuse. Another argument could be made for banning for-profit hospices.
As a community, we have a lot skin in the game. Many of AAHPM’s members and leaders work for for-profit hospices, including the current president, the medical director of Gentiva, the nation’s fastest growing for-profit hospice provider. Many others work for Vitas. Amusingly, Vitas, the nation’s largest provider of care to the terminally ill, is owned by Chemed Corporation, whose other holding is roto-rooter, the nation’s largest plumbing and drain-cleaning provider.
As these arguments play out in the press, congress, and the courts, we should try to sharpen our message as a community about the role of profit in the hospice industry. The risks of not thinking this through and letting others craft the message are too great.
by: Alex Smith



