Acute Care for Elders (ACE Units) have been around for over a quarter of a century. Randomized trials of ACE units date back to 1996 when Seth Landefeld and colleagues published a study in NEJM showing that they improve basic activities of daily living at discharge and can reduce the frequency of discharge to long-term care institutions. But if ACE units are so great, why do so few hospitals have them?
On today’s podcast we talk about ACE units with geriatricians Kellie Flood and Stephanie Rogers. They recently published a paper in JAGS looking at the current landscape of ACE units in the US. In the podcast we go over these issues and more:
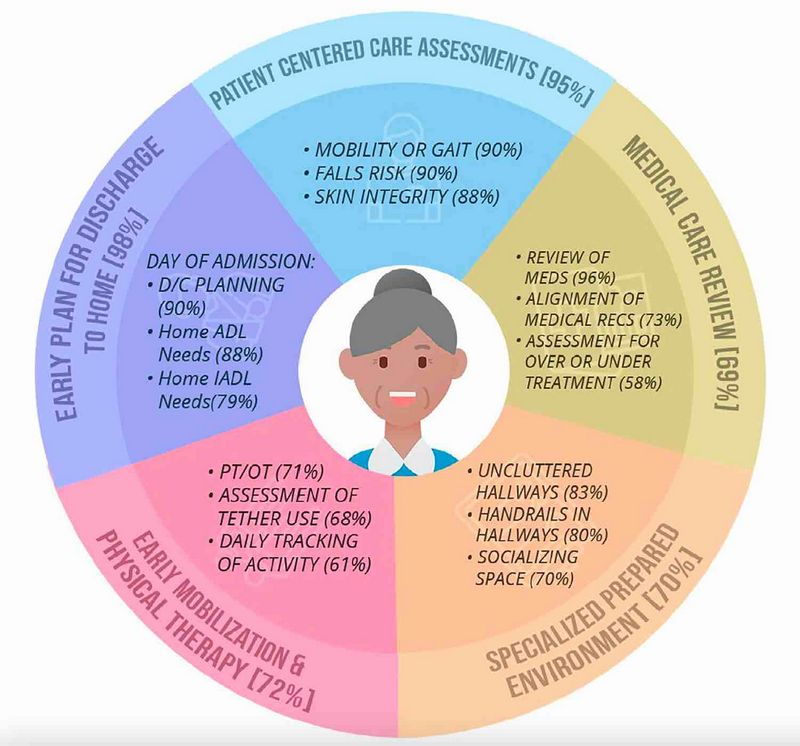
- What are ACE units and what structural elements go into them (see the picture below for a nice summary)?
- Which patients are eligible to go to an ACE unit?
- What are the benefits of an ACE unit?
- If ACE units are so great, why are they not so common?
- What does the future look like for ACE units and how does it differ (if at all) from Age Friendly Health Systems?
If you want to do a deeper dive in ACE units, check out some of the following articles:
- The original NEJM paper on ACE units from 1996
- Kellie Flood’s paper in JAMA IM showing that not only ACE units deliver better care, but also help with the hospitals bottom line
Eric: Welcome to the GeriPal Podcast. This is Eric Widera.
Alex: This is Alex Smith.
Eric: And Alex, who do we have with us today?
Alex: We are delighted to welcome to the GeriPal Podcast, Kellie Flood, who is a geriatrician at the University of Alabama Birmingham and associate Chief Quality Officer for Geriatrics and Care Transitions. Kellie, welcome to the GeriPal Podcast.
Kellie: Thank you so much. Great to be here.
Alex: And we’re delighted to welcome back to the GeriPal Podcast, Stephanie Rogers, who’s a geriatrician and medical director of UCSF’s, age-friendly health systems. Welcome back, Stephanie.
Stephanie: Thank you. And I’m delighted to share a podcast with my mentor and friend, Kellie Flood.
Eric: And we’re going to be talking about improving hospital care for older adults via ACE units, or acute care for elders. But before we do, do you have a song request? I think Kellie, do you have it?
Kellie: Our fabulous song request actually came from Stephanie Rogers.
Eric: Stephanie Rogers. Got that one wrong.
Stephanie: Yeah. So I picked the Ed Sheeran song, The A Team, because it reminds me of our ACE team that goes around the hospital and cares for our older patients.
Eric: Are you an Ed Sheeran fan?
Stephanie: I don’t know too much of this stuff. I do like this song though.
Alex: Yeah. So then it’s a great choice because of the title of the song, though the content is about a prostitute who’s down on our luck and living on the streets. But we’ll get the title in there, it’s good enough. That’s great. All right, so here’s a little bit of that one.
(singing)
Kellie: Great job, Alex.
Eric: Excellent song. So let’s dive into the topic, ACE units. I’d like to talk a little bit about what they are, do they work and are they like the song where maybe they’re a little bit down on their luck, like Alex said, right now? Or are they doing really well? So before we get into that, ACE units have been around for over 25 years. My past boss, Seth Landefeld, wrote a Seminole paper on this back in 1996 in the New England Journal, showing that ACE units improved things like ADLs at discharge, discharged to long-term institutions. Kellie, why did you get interested in this as a focus of your academic career given that they’ve been around for so long?
Kellie: And just to demonstrate what a small world we live in, Seth Landefeld is my current boss. So we really have come full circle.
Eric: All roads lead back to Seth.
Kellie: That’s right, that’s right. Especially all ACE roads. Seth and many others. And I also want to commend my, who I would call also peer mentor and I follow and learn from Stephanie Rogers for even doing the study that we’re going to talk about that she led in the first place. So as I was a geriatric fellow in my one year fellowship, I was introduced to this thing called an ACE unit because my home institution at that time was developing its first ace unit. And ACE units in general take a typical multidisciplinary hospital unit that has all the different team members, so doctors, nurses, social workers, dieticians, pharmacists, chaplains, patient care technicians, others I’m leaving out. And in the traditional hospital models, all those folks are coming to work and working hard every single day.
But we’re trained in our silos and we tend to practice in our silos and our primary means of communicating with each other may be in the chart in the medical record. There may be some occasional conversations between doctors and social workers or maybe between doctors and pharmacists, but it’s not in the traditional hospital model for all those folks to get around a table at the same time. And also to have those folks proactively assessing and addressing geriatric syndromes. And that’s what an ACE unit does. It converts a traditional multidisciplinary team into an interdisciplinary or interprofessional team that is trained to assess for and address risk factors for or existing geriatric syndromes that our older adults bring to the hospital with them. And that model just made sense. After coming out of residency and taking care of lots of complicated older adults as of now, a brand new physician attending, I really needed that team to help me out. So it just seemed to make common sense and I’ve really been sort of hooked on the model ever since. And I’ll pause there and see what Stephanie has to add to that.
Eric: Yeah, when did you get hooked, Stephanie?
Stephanie: Yeah, I agree. I was lucky to work on two different ACE units in my geriatrics fellowship. They were run very differently but had the same concepts. And a light bulb just went off in my head, like, yes, this makes sense as a model for how we should care for more complex older patients. And I loved working with the interdisciplinary team. I loved focusing on these other issues that are very important to older adults, like their function and their social circles and medications and all these other things that you normally don’t focus on. And yeah, it just clicked for me like yes, this is how I like to practice medicine.
Eric: Maybe we can take one big, big, big step back and just talk about Kellie, you’ve briefly touched on what is an ACE unit. So ACE stands for if I’m correct because I’m terrible acronyms, acute care for elders unit, right?
Kellie: Yes.
Eric: And I loved in your article that you wrote in JAGS, which we’ll have links to in our show notes, you have a beautiful diagram figure that we’ll also include on our website for the key components for ACE units. What are those key five components?
Kellie: Yeah, so the core components, which I was very happy to see that the study demonstrated, there’s still a lot of fidelity to these five core components of an ACE unit is what I mentioned before, is this really structure and process that allows for this patient-centered assessment focused on geriatric syndromes, originally around function and predominantly around function and cognition and again, sort of related outcomes such as nutrition and continence and pressure injury. So that’s one, this patient-centered geriatric assessment and management approach.
Number two, a structure that allows for daily review of a medical plan of care to make sure number one, it’s not harmful and make sure it’s goal aligned or goal concordant with what these vulnerable older adults want. And that’s to include making sure we’re using safe prescribing practices.
Number three, this specialized prepared environment that promotes safe mobility and cognitive stimulation and delirium prevention, so sort of environmental changes. Number four, again, structure and process that promotes early mobilization which may or may not require a formal OT and PT consultation. And then number five, really proactive care transitions planning out of the gate on day one.
Eric: And Stephanie, you come from a unique perspective because you started an ACE unit at UCSF. Were all of these things being done already? How much of a lift is it to do these five things and to create this ACE unit?
Stephanie: Yeah, I think that is what’s interesting and what drove me to start thinking about this paper was that when you start an ACE unit, you have to start it in a unique environment. Not every hospital or every health system is the same physically or financial incentives or which clinical programs exist and patient demographics. And so how can we adopt these five elements for the unique environment that we’re in?
And I found that I had to actually just call around to friends and mentors across the country who had ACE units and ask questions, “How do you do your interdisciplinary rounds? What is your clinician to patient ratio? How do you guys assess for delirium?” And the environment that we worked in, in geriatrics, was more of this sharing information and different groups or calling. And I thought to myself, wouldn’t it be great if we could just understand first of all how many ACE units there are in the country, but also how are they doing these five elements in their unique environment so that other people who perhaps want to start an ACE unit can read this paper and get ideas of the many different ways that you could have these five elements in your environment.
So that was sort of how I was thinking about it. I spent so much time trying to talk to others to find out this information. I thought it would be great to just put it all in one place.
Eric: And particularly, the one that seems the hardest is changing the physical environment. In some ways, I mean it’s hard because you got to change it. But in other ways, if you look at Seth Landefeld’s New England Journal study, a lot of the things that were done in that original study seem a lot more common now, like handrails, less cluttered hallways, large clocks, calendars in the rooms, thinking about things like how do you get in and out of a door, toilet seats, things like that. So in some ways it’s great because some of this is diffused throughout the hospital environments everywhere, but there’s probably other things that you want that are really hard to change without a lot of money.
Kellie: Yeah. I really appreciate you saying that and really highlighting that because I too reflected on the findings from the paper and just observations that I think it’s a great positive sign of the impact of ACE units and the fact that so many things written about in that paper are now just commonplace. I’ll say sometimes this is also the heaviest lift because it’s the part that costs money, right? Because when you’re really converting the team, you’ve got all the people you need working on the unit for the most part. And so there’s not a lot of added cost. Yes, you need some protected time for leaders to provide training and structure and oversight and ongoing quality assurance, but the heaviest sort of cost lift sometimes is redesigning the physical space. And so for our example, when we launched our brand new ACE unit here at UAB in 2008, we did not have the funds to redesign the unit until three years later.
So we didn’t want perfection to get in the way of progress when we knew we could already positively impact the experience and outcomes for our patients and our team members by putting the team together and building up the team while we were continuing to set the conditions and number one, identify what environmental modifications we wanted to make. So it gave us time to put that interprofessional expert team together. And then when the timing was right, we were actually able to move to a side of the hospital that had bigger rooms and then redesign that unit. So there was some advantage in going ahead and launching our team and everything else and not being frustrated by having to wait for the environmental changes.
Stephanie: And Kellie, actually that’s one of the things that I remember you teaching me was you just said, one day we just called ourself an ACE unit and we didn’t really have many of the components yet, but we slowly built them over the next year or two. But this day, we called ourself an ACE unit. And I thought that was so helpful when we started ours because we did the same thing.
Eric: That’s the same thing me and Alex did with podcasts. We just called ourselves podcasts.
Kellie: You can’t get stuck in analysis paralysis, right? And so we had spent a year with all the senior stakeholder engagement and support and the leadership roles and things like that. And then we had half day workshops to get the frontline team just really excited about being the first ACE unit in the State of Alabama. And then we set the date for that first interprofessional team meeting. I brought in the bagels, people showed up and we were off and running after that.
Eric: I briefly touched on Seth’s paper, but what do we know about the evidence for ACE units? Do they work?
Kellie: So the nice thing is about having 25 some odd years go by is it’s now a no doubter, right? So there’s been plenty of studies that have evaluated and confirmed that the ACE unit’s original intent still is still a benefit, that you can preserve functional independence or reduce functional decline. I think what those who work in the space have done a great job is also expanding and demonstrating all the related and cascading benefits. So delirium reduction, like the stay reduction, reduce readmissions, reduce cost of care. And especially those cost and return on investment evaluations are even more important I think today than perhaps in the past.
Eric: And you’ve done that, right? JAMA IM 2013, you had a paper that showed what, 300, $400.
Kellie: It’s really interesting because our ACE unit formally launched in, we had our first fiscal year’s worth of data that I was, long story short in development, one early lesson I learned is always partner, identify your C-suite stakeholder owner who’s going to benefit from this work and partner with them. So I was partnered with my vice president and we were doing just return on investment analysis to report back internally.
And the more we started looking at the data, the more it kind of dawned on me, I wonder if this is worth writing up too. And thankfully, I have fabulous mentors who said, “Yes, you should write that up.” And so it didn’t start out as a publication, it started out as what had been our yearly report back to the organization on return on investment. And essentially demonstrated that even with very short lengths of stay in your ACE unit versus our control unit, you can reduce cost of care and it’s likely from delivering gold concordant or more appropriate care. And then a surprise finding was even with the length of stay of about four, four and a half days, we saw a reduction in 30 day readmissions.
Eric: Wow. So it looks like they work. Stephanie, you decided to do a JAGS paper, just published in JAGS I think mid of last year, looking at where we have ACE units in the US and what does that landscape look like? Why did you decide to do that paper?
Stephanie: Well, as I talked to people across the country, it seemed to be always the same people. I knew the same people that had the same ACE units, but I was curious if there are ACE units other places. And there was sort of this quote floating out there that there are 200 ACE units in the country. And I kept trying to find where this came from but couldn’t find it. And so I thought let’s try to figure out actually how many they are, where they are they in academic centers and community centers. And the goal is to maybe just form a community of people so that we can learn from each other. And so that’s where we started was just sort of figuring out where these ACE units are. And unfortunately, we were quite surprised because we found 50 ACE units that we think have or had existed at some time. And then 43 of those ACE units actually filled out our surveys so that we understood what was going on in their ACE units. But only 50 ACE units out of the 3,600 hospitals that exist in the United States.
Eric: 50 out of 3,600?
Stephanie: Yeah. So we never got close to that 200. Yeah, couldn’t find them.
Kellie: And I think the lesson that Stephanie taught me in that, or the reminder is we have this internal saying here within UAB that we’re going to make data driven decisions, we’re not going to operate on anecdote and folklore. And Stephanie’s study was a reminder that the ACE community, I don’t know where this number of 200, but I’m a person who was repeating that number as well. So it was one of many reasons why this study needed to be done. And again, huge kudos for Stephanie for taking the lead and to get the ball rolling.
Alex: One question about that number. If you had a university system that has three hospitals, each of which has an ACE unit, does that count as three ACE units or does that count as one ACE, that counts as three ACE units?
Stephanie: Yeah. We contacted every single hospital in the country.
Eric: So our UCSF ecosystem accounted for three of those 43 active ACE units?
Stephanie: Yes.
Eric: I want to dive more into this, but I kind of want to ask the question. I’m going to turn to you, Kellie. If all of this evidence suggests that ACE units are so great, why are they so uncommon?
Kellie: Yeah, so that is the $64,000 question that Stephanie and I have been pondering and chatting about since these findings. And I’d love to hear what the entire group’s thoughts on are this. I think some of my thoughts are informed by some of the responses we got back on the survey around if you’d had a ACE unit and it had closed, why was that? And then also some of my thoughts are informed by being contacted from health systems across the country over the years who wanted to start an ACE unit. And I think one of those is you have to have a local champion with some content expertise and there’s just not a ton of geriatricians running around. And those that are out there in this space tend to be grouped together in academic medical centers. And so we have thousands of hospitals that aren’t academic medical centers.
I think the other discussion point is, and we worded it in the paper this way, this perceived lack of financial incentive or return on investment when actually there’s great evidence of fabulous return on investment. So I think the opportunity for the field is how can we equip those content experts that are out there to better communicate the return on investments? And that’s where we spent the bulk of our time and effort here at UAB is around developing that skill and that requires constant communication. So I think those are some initial thoughts that I’ve had and I’d love to hear what everybody else thinks as well.
Stephanie: If I could add on that financial piece, I had to spend a significant amount of the first couple years of my career learning business. I went through medical school and I learned clinical medicine, but all of a sudden when I was talking to our C-suite leaders or the people who were going to support this program, they spoke a different language that I didn’t understand. And I had to learn that language and I had to learn how to frame things in the way that they cared about. And so Kellie always taught me to ask people, “What keeps you up at night? What are you worried about?” And I started to ask those sorts of questions. And even though ACE students have been shown to have great clinical outcomes like decreased hospital harms, yes, health system leaders care about that. But also they really want to know about the bottom line.
And so I can say it has all these great clinical outcomes, but I would highlight the things like decreasing length of stay and readmissions and decreased costs and so those sorts of things. And so I started reframing the way that I was talking about ACE units. And that was something that I didn’t learn in my career as a doctor. And I think that’s where we sort of fall short as geriatricians or hospitalists or nurses, whoever’s implementing these geriatric models of care. You have to learn an entire different industry in order to be successful at sustaining these types of programs.
Alex: I think there’s an analogy here to palliative care and the explosive growth of palliative care in US hospitals. And why is it that ACE units haven’t seen a similar explosive growth in US hospitals where the majority, I think it’s over 80% of major US hospitals, large US hospitals have palliative care service at this time? Just gigantic. And it’s something like 50% of the smaller size hospitals. And I think that there are a few reasons for that. One is that there was a clear financial case for expansion of palliative care and I think you could say, well there’s a clear financial case for expansion of ACE units.
And the second is it kind of builds on what Kellie was saying about champions, but it goes beyond that in that the, there’s a national organization called the Center To Advance Palliative Care, or CAPC, whose mission is to advance the practice of palliative care nationally. And there may be some similar geriatrics organization. I don’t think AGS is quite that because it’s the professional society. That’s more similar to AAHPM or HPNA on the palliative care side. But I don’t know that there is, I’m interested to know is there some equivalent organization that promotes… I doubt it because otherwise, you probably would’ve had an easy source to go to in order to identify existing ACE units. But thoughts about that, Kellie and Stephanie?
Kellie: So I love where you’re going Alan because Stephanie and I have also talked about this. So UAB is a CAPC training site and when I was recruited to UAB hospital to start an ACE unit and I had the great advantage and good fortune and blessing in that our UAB hospital palliative programs were about four years ahead. So I just copy and paste, the processes and steps and the business case they met made to start their inpatient powder programs here I just applied to ACE unit and other geriatric programs.
At the same time, I have since seen our palliative team through CAPC train 89 other health systems in launching palliative care programs. So I think the geriatric world has parts of what CAPC offers. So these health systems who engage to develop palliative programs, they pay a fee, so they’ve got skin in the game, and they get a very intensive onsite training and ongoing coaching that all together, I think in the geriatric side you sort of have to piece some of that together. So you can reach out to a Stephanie and get perhaps onsite training at UCSF, but Stephanie doesn’t have the bandwidth and Kellie doesn’t have the bandwidth to provide the level of coaching and mentorship that’s really needed that a health system can get through a CAPC, but they’re also paying several thousands of dollars to invest in developing that. So I don’t know if that made sense or Stephanie, what else you would add to that.
Stephanie: Yeah, I think you said everything. And Kellie and I have talked about what would it take to start something like that and it’s obviously a very big lift.
Eric: Can I also dive into the results of the paper a little bit? Because you have some data on the makeup of ACE units and kind of what components that they cover. What are the team members for these ACE units?
Stephanie: Yeah, there’s lots of varieties of what people do with their interdisciplinary teams. So one thing we asked is how do you do interdisciplinary rounds? And the majority of ACE units actually have the members sit in an extra room and kind of talk about patients. But there’s other ACE units where they round at the bedside or they round on Zoom, this was pre COVID, or they have a checklist that a nurse fills out and someone else reviews. So there was lots of permutations of how people did rounds.
And then within those interdisciplinary rounds there were differences in who was at rounds. Most ACE units had the bedside nurse, the physical therapist, a social worker, a case manager, and then differences in a lot of other people, chaplains, nurse practitioners, the primary teams. So there was a lot of difference in who was at these rounds. And that makes a lot of sense to me because when we started our ACE unit here at UCSF, I had to go around to all of these different disciplines. And like Kellie was saying, yes, all of these units already have all of these disciplines working on a unit, but they’re not working in a coordinated way. So can I get the physical therapist who’s billing for visits all day long to actually come sit in a room and listen and talk to the interdisciplinary team? What effect does that have on the bottom line? Same for the nutritionist and the chaplain and all these people. So there is a lot of negotiation and restructuring of how people work in the hospital to figure this out. And so again, I think it’s unique for every environment
Kellie: And that is why engaging and obtaining not only really buy-in, but ownership from each of those interprofessional department leaders around the return on investment so their physical therapists can be freed up 30 minutes to sit in.
Eric: Did you ask who’s eligible for ACE units? Is it all older adults? Frail older adults? Older adults over certain age?
Stephanie: Yeah, we asked who do you choose to be on your ACE unit? I think around 80% of the ACE units actually had an inclusion criteria, and then 40% had an exclusion criteria. The most common criteria was obviously age. And I think 65 and up was the most normal, was the most common age cutoff. And then there was other things. Are they community dwelling? Which is who a students were intended for in the original RCTs. And then there was different exclusion criteria as well that people had. So was the patient, didn’t have the ability to improve function or maybe they were completely dependent and so maybe they weren’t the best ACE patient. So there was all kinds of varieties of what people included. It sounded like too, an ACE unit is a specific unit in the hospital. And in some ACE units, that entire unit is ACE patients. In other ACE units, some of that unit is ACE patients and the rest of the unit is other med-surg patients. And so even just the physical way that the unit was laid out was different among different ACE units.
Alex: Did you specifically ask about mobile ACE units or do you assume that those who didn’t have a physical, I think it was about 70%, had maybe their own location and that the other 30% or so were mobile units?
Stephanie: Yeah. We actually asked in the survey about mobile ACE units, virtual ACE units, all the different kind of varieties of this and we just felt like it was out of the scope of this paper. But we do have information on how many of those exist and a few details about how they run as well.
Kellie: And I think this discussion really again points to a strength of the ACE model is yes, you want to adhere to the core elements so you can achieve the desired outcomes and also, they can still be nimble and adapt to the needs of your organization, and again, allow us to not get in analysis paralysis, but to continue to make progress even if it’s not exactly the way it was done at UAB or at UCSF. What meets the needs of your organization?
So for example, we can’t have a lot of admission criteria because we’re always in a bed capacity crunch. So what meet the needs of our organization is we successfully have on our 25 bed ACE unit on any given day, 20 of those patients are 65 and older. But we’re not going to have angst around the 40-year-old that then bed two. Number one, it gives our nurses a little bit of a break to have someone who can walk and doesn’t need total care. And also, it meets the needs of the organization to move that 40-year-old out of the ED into the bed.
Alex: Yeah. I want to ask also about something we said a couple questions ago about the composition of the multidisciplinary team, focusing in on the ACE attending. 81% had an ACE attending. Interesting to know what the other 19% had. And of those attendings as 80%, 44% hospitalists, 23% geriatricians, and 33% mix of hospitalists and geriatrician. That surprised me. I have to say I thought it was going to be mostly geriatricians, but it’s actually mostly hospitalists. So any comments about that?
Stephanie: Yeah, I was also surprised by that. And unfortunately, we don’t have a lot of details of what that looks like. Is this an institution that has one geriatrician and has trained a bunch of hospitalists? I don’t know Kellie, I know you’ve done a little bit of work around this, maybe you have a better idea.
Kellie: Yeah, yeah. I appreciate it. So I too was encouraged by this. I think that it helps us around scalability to the model when we just don’t have enough geriatricians for every hospital to have a geriatrician. So we’re an example of an ACE unit who has never had the geriatricians as the attendings because even here at UAB, we’re rich in geriatricians compared to every other hospital in my state. I don’t have enough geriatricians to be the attending of record. And until the last year, I’ve not even had a geriatrician really operate on our ACE unit for the past four years. So our ACE unit out of necessity and in the spirit of progress, our hospitalists are attendings and we’ve really robustly trained geriatric nurse practitioners to be the geriatric content expert in the ACE rounds and doing consultation on our more complicated patients. So I think it again, allows for a way to scale the model to have more reach.
Alex: On the one hand, I like the positive spin you’re putting this. On the other hand, I’ll say that within palliative care, the explosive growth of palliative care consultations in US hospitals has also been coupled with the sun setting of being able to be a fellowship trained… You have to be a fellowship trained palliative care doc in order to be a palliative care provider in many of these institutions. And that’s driven opportunities for training palliative care clinicians. And our palliative care fellows get multiple job offers from multiple hospitals because they’re looking, they’re hungry for these. And I don’t see the same demand in geriatrics. So while I appreciate that the model’s flexible and that hospitalists can serve in this role and that creates opportunity for geriatric nurse practitioners, I also worry that it may be a missed opportunity to drive growth of geriatrics, which we know is a somewhat either stable or constricting profession.
Kellie: Yeah, totally agree. Yeah, yeah. So to try to address that, here in Alabama we are making progress in sort of this hub and spoke approach to try to close this gap. So a real life example, we have identified a partnering rural hospital here in Alabama who we’ve engaged their C-suite, they’re absolutely fabulous and they desire to be the exemplar rule, hospital age-friendly health system. So they identified a local internist who they are supporting to come to UAB for a year. He is in our geriatric fellowship and will return to be that campus’s only geriatrician for now and will launch all of their age-friendly health systems. So if UAB is the hub, they’re a spoke into a rural health system. That rural health system is connected to osteopathic training programs who will now have exposure to a geriatrician who we would love to recruit into our fellowship and then send to other rural hospitals in Alabama because that’s where they work anyway.
And so that will be an active intentional work once he finishes our fellowship this June to go back and create that pipeline. At the same time in our Huntsville branch of our University of Alabama system, we have their first ever hospital-based geriatrician. Their Stephanie, who’s been there one year, so that’s another spoke to a 900 bed hospital. That hospital has several affiliate hospitals. So their Stephanie is now launching their consult service and perhaps eventually their ACE unit, who will then reach into their affiliate. So we’re trying to aggressively close that gap through this hub and spoke approach and methodology and are now seeing some progress in that.
Alex: Great.
Eric: And quick question, Kellie, do you train all the hospitalists around geriatric principles who attend on the ACE unit?
Kellie: So ideally, yes. There’s been some challenges around that. So we really work to redesign the system. So the system drives the providers to deliver age friendly care.
Eric: Okay. I also want to talk about the future of ACE units. Now, is the future, you mentioned age friendly health systems, the average daily census, Stephanie you found was 18 patients for these units. I’m guessing the hospital size is more than 18 patients and the majority of hospitalized adults are older. So is the future of just redesigning the entire hospital, be age friendly? Is there a role in the future for ACE units if that occurs? Where are we going with all of this? How do these age friendly health systems and ACE units fit in together? Great. I’m going to Stephanie first on this one.
Stephanie: Yeah. And Kellie and I talk about this all the time and we use the same hub and spoke idea within a health system. So I think that the ACE unit and what we learned from a lot of these ACE units that we surveyed, there is sort of this hub of education and hub of training and hub of QI system changes that goes on within their ACE unit that then disseminates to other units throughout the hospital, even clinics, post-acute partnerships they have. And so I do think there is a role for ACE units to sort of be a hub within a hospital or a health system for geriatrics education and training in QI and even research and that the other units can become age-friendly from learning from this specific area. And we do know there are older patients that are more complex than others and maybe they would benefit from a more intensive ACE unit like environment that has all these five components. And there’s other adults, older adults, that could be on other units that could get some of these more systemic geriatrics changes.
Eric: What do you think, Kellie? Any other thoughts?
Kellie: Yeah, I agree. I have a colleague here who leads our clinical practice transformation department, so our performance improvement department who is fabulous and sort of counsels, we don’t want to set the bar low or lower than it should be. I feel like the ACE unit model has proven it is the gold standard. Now balancing that with all the things we’ve already talked about that we can’t let perfection get in the way of progress and there’s just very real life challenges and barriers. There’s reasons why we only found 43 active ACE units. So I think it’s somehow striking this balance that the ACE unit is the gold standard and also, it’s encouraging that over 2,700 of health systems have engaged in that age friendly movement. So if you can’t do an ACE unit, make progress. And the ACE unit processes provide the blueprint on how to make progress.
Eric: So can I ask also, Stephanie, you did this survey fall of 2020. Now if memory serves me correct, there was a pandemic going on then. So two questions about that. First is, do you think that affected the number of ACE units that are out there? Because there is a lot of shifting wards into COVID wards and everything else. How are you thinking about that?
Stephanie: Yeah, in our survey we asked everybody to answer the questions as if it was pre COVID because we know a lot of things changed in COVID. But also, I’m not sure it changed the overall number because our initial question was, have you ever had an ACE unit at your institution? And I can’t remember the exact number, but the majority have closed only recently. Some were open for many years. I’m not aware of any ACE units that closed because of COVID. I know a lot of changes happened and the infrastructure, but I’d be curious to know what’s happened now, three years later.
Kellie: I do think it might have impacted our response rate, yes. So I think around half of the hospitals actually responded to the survey. So it is it possible that some of those hospitals who never responded also have an ACE unit? I’d like to think yes, that’s possible.
Eric: Getting closer to your 200 number there. Another question is, man, it feels like our response to COVID was anti-age friendly care in the hospital, isolation, especially early on. Again, just trying to figure things out, so no judgment. People were getting loads of medications we wouldn’t otherwise give. How has COVID affected ACE units, do you think?
Kellie: For us, this ties back to your question around ideally we would be training our hospitalists who work on our ACE unit. Our hospitalists were taking care of COVID patients. And up until recently, because of lack of geriatricians, I didn’t have anyone to train the hospitalists. And I think in a lot of ways, I know our ACE unit is almost restarting in a lot of ways. The good part about that is we get to start afresh. Our hospitalists have pretty much turned over, my inpatient geriatric team is largely turned over. We can take all the lessons learned in the past and sort of start out ahead and start afresh and then take some things that we came out of COVID, such as Zoom, and better connect with team members who maybe can’t travel all the way to where our ACE unit is. So I would suspect we’re not alone in the ACE unit world of having to do a reboot or a restart, but it’s a more informed, I would say, reboot or re-imagining.
Stephanie: Yeah, the exact same thing is happening here. I feel like we’re starting over and a lot of that is we had group activities like what we called ACErcise and what are the rules around that now that every patient has to be masked in the hallway and who can come out of their room and be with other patients. All these rules have changed. And so we had to redesign all these things. And we didn’t have volunteers for a long time and now we’re slowly bringing back volunteers to visit our patients so they’re not isolated. So there’s a lot of doing everything over, but it is an opportunity to rethink how we do things.
Eric: Great. Well I’m going end with one last question. You got a magic wand. You can do one thing with that magic wand to improve care for older adults in the hospital, Steph Rogers, what would you do?
Stephanie: I think I would work on system changes that really make it easy for clinicians and people of other disciplines to do the right thing, caring for older adults because we don’t have the time to, everybody to get hours and hours of education. Can we set up systems that allow them to make the right choices in caring for older adults?
Eric: Kellie Flood?
Kellie: I would agree with that. And couple that with aligning perhaps policy or regulatory, in a good way, incentives for health systems, for all health systems to see the benefit or the need or the desire to transform into age friendly health systems. So whatever support an alignment around incentivizing health systems to.
Eric: And does that age-friendly health system include The A Team?
Stephanie: It does.
Eric: Alex, that’s your cue.
Alex: All right, here’s a little more.
(singing)
Eric: Kellie, Steph, thanks for joining us on the podcast.
Stephanie: It was great. It was lots of fun.
Kellie: Thank you all so much. Really appreciate it.
Eric: And as always, thank you Archstone Foundation and to all of our listeners for supporting the GeriPal Podcast.



