If you happened to read WebMD the other day you would have seen an article with the headlines ‘DNR Orders May Affect Surgical Outcomes’. This is a fair enough title, as the topic of the article is a recently published manuscript from the Yale School of Medicine that concludes that do-not-resuscitate (DNR) status appears to be an independent risk factor for poor surgical outcome.
At issue though is not the title though. It is the lack of a good understanding of what was actually published in the Archives of Surgery paper and the significance (or lack thereof) of the research results. As a prime example of poor reporting on this particular paper and the harm that may from it, I’m going to start off with the second paragraph in the WebMD article:
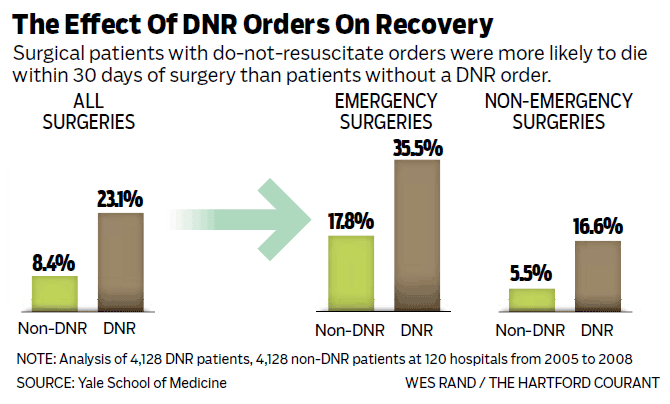
“A new study shows 23% of people with DNR orders died within 30 days after surgery compared with 8% of similarly matched surgery patients without DNR orders. They were also more likely to suffer serious complications and have longer hospital stays.”
Sounds pretty convincing. I mean they were ‘similarly matched’, right? Well, lets take a closer look at the Archives of Surgery Article.
The authors did a retrospective analysis of 4128 individuals with a pre-existing DNR order who underwent surgery at more than 120 US hospitals participating in the American College of Surgeons National Surgical Quality Improvement Program (ACS- NSQIP). They then found 4128 age and procedure-matched non-DNR patients as a comparison group. (An individual was deemed to have a DNR order if it was signed in the patient’s chart in the 30 days prior to surgery or if there was a DNR order but it was rescinded immediately prior to surgery).
Can you guess what you find if you match DNR to non-DNR patients only by using age and procedures?
Well the first thing you find is that matching only by age and procedure gives you a very poor match (I know – shocking). DNR patients were more likely to be admitted from somewhere other than home, had functional impairment, had a quickly worsening functional status between illness and surgery, had abnormal preoperative lab values, worse ASA class, had an inpatient procedure, had contaminated or dirty operative wounds, and had an emergent procedure. DNR patients also had more comorbidities (mean of 4.3 comorbidities vs 3.1 comorbidities for non-DNR patients).
The unadjusted outcomes reveal a very novel finding – sicker patients have worse outcomes that those who are not so sick (that’s how I would have titled my WebMD article). The sicker DNR patients (labeled as DNR patients in the study) had higher complication rates than non-sick patients (labeled as non-DNR patients). DNR patients were also more than twice as likely to die within 30 days of surgery (see table). The authors report some other unadjusted outcomes, but it’s all pretty useless given that the two groups are so very different.
The authors did attempt to adjust for multiple significant risk factors. After adjustment, a DNR order remained an independent risk factor associated with death (adjusted odds ratio). What are we to make of this? It is possible that physicians were less likely to provide life-prolonging treatments unrelated to CPR to DNR patients resulting in a higher mortality. It is also very likely some other unmeasured aspect accounted for the higher mortality, including that the DNR group may have had different goals than the non-DNR group when it came to to other life prolonging treatments.
So, what’s the take home message? The study gives us evidence that individuals with DNR orders are more likely to die at 30 days than those who do not have DNR orders. However, as Ken Covinsky wrote in a previous comment on opioids and fractures, “it provides meager evidence” that DNR orders are the cause of the higher mortality.
by: Eric Widera (twitter: @ewidera)



